Tag: doctor
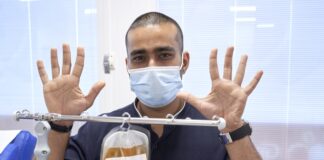
PLASMATASTIC! Covid surviving Doc saving lives through his blood!
A medic who survived the coronavirus is saving lives in more ways than one - this time through the plasma in his...
Top Doc! Bradford clinician who set up one of world’s largest...
A clinician who played a leading role in responding to the Covid-19 outbreak in Bradford and set up one of the world’s...
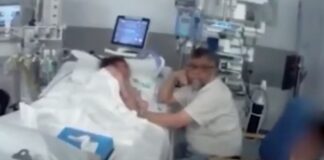
SHOCKING: Footage of father being dragged away from dying daughter’s bedside...
Shocking footage has emerged of the moment a father was dragged away from his dying six-year-old and arrested after being told she...
TV doctor reminds us of the ways we can celebrate Eid-al-Adha...
GP, television doctor and author Dr. Amir Khan features in a new video for the government which acts as a reminder on...
A stiff fine: Doc having affair admits prescription fraud for free...
A court heard how a married fertility consultant wrote fake prescriptions to get packs of free Viagra to boost his performance in...
SLUM-DOC: Miss England & NHS medic to host online fundraiser
Britain’s beauty queen and medic, who returned to England to rejoin her post as an NHS doctor, calls upon the public to...
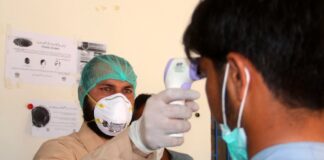
Pakistan: May reinforce lockdown after spike in infections
Pakistan may reinforce its lockdown to stem the spread of the coronavirus, officials have said, amid a spike in infections and...
COVID survivor says going home was best birthday present EVER
COVID-19 patient Khurram Khan got the best birthday present he could wish for - going home from hospital with his family after...
Ten UK doctors have died from coronavirus. All were immigrants.
In a country where anti-immigrant sentiment gave rise to the Brexit movement, and almost fifty percent of all hate crimes reported have...
Miss England returns to Britain to resume NHS job as doctor
“I’m a trained doctor - my services would be much more useful in a hospital," Bhasha Mukherjee says.
‘Terrifying’: Doctors alarmed on lack of protective kit for dealing with...
British doctors and health workers throughout the UK have voiced alarming concerns about a lack of sufficient Personal Protective Equipment (PPE) to...
Woman receives suspended sentence for causing death of Imperial College ...
A woman has been given suspended sentence for careless driving, which caused the death of a doctor who was on his daily...
“Master of Deception”: London GP jailed for 90 sex offences
A general practitioner has been jailed for at least 15 years after being convicted of 90 sex offences against 24 female patients.
Batley GP selected as new chair for CCG
NHS North Kirklees CCG has announced the appointment of Dr Khalid Naeem as their new clinical chair of the governing body from...
Doctor convicted of sexual assault offences against patients
A former doctor has been found guilty of sexually assaulting dozens of female patients by conducting unnecessary, intrusive medical examinations over a...
GP’s stand up for Grenfall: London-based doc-turned-stand-up-comic raising money for tower...
Ahmed Kazmi played two sell-out shows in Notting Hill with his act 'Doctor in the House: what your doctor really thinks' and all the...
Leeds doctor shares a secret spy’s insight into life on the...
999’s answer to 007
After last week’s demonstrations in Leeds against NHS reforms, one of the biggest protests the city has seen in years, thousands...
Gaza doctors return
Volunteers complete selfless work in war-stricken region
A group of UK-funded NHS surgeons have returned from treating war-wounded patients in Gaza six months after the...
Highest honour for BRI doctor
A doctor from Bradford Royal Infirmary said he was ‘incredibly humbled’ after learning of the news that he was to be honoured with his...