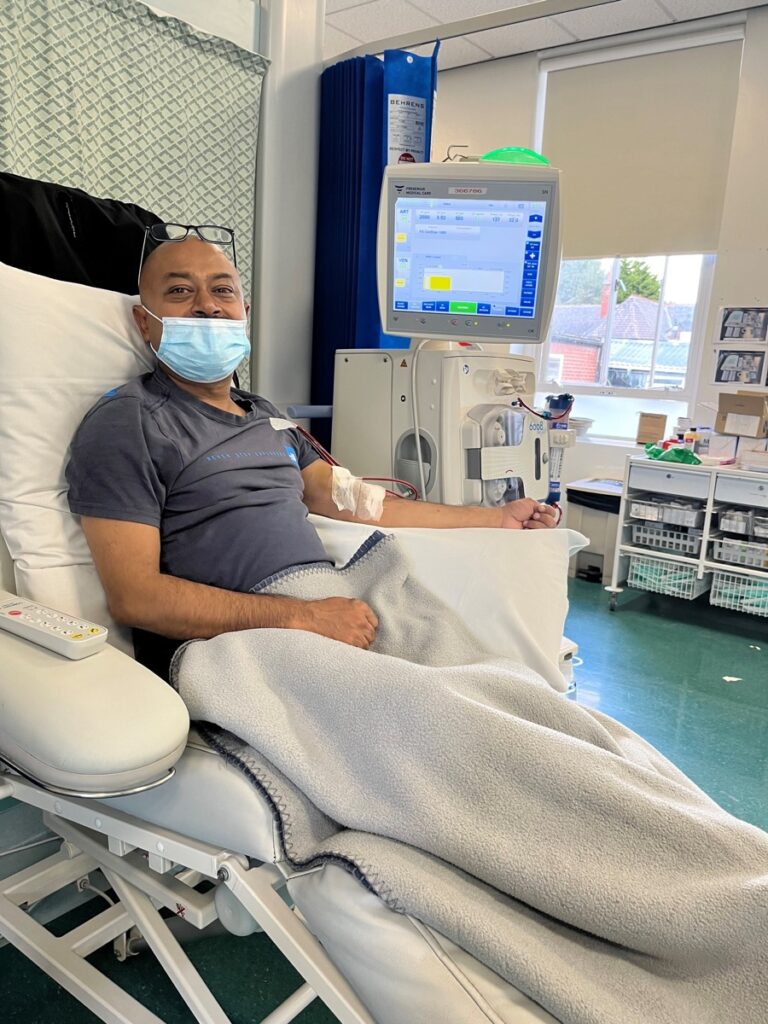
Min Minhaj, 48, from Calverley in Leeds has been on the kidney transplant waiting list for over three years, and says that his life has tuned into endless hospital appointments, and fears his dialysis might stop working.
Around a quarter of some 4,744 patients on the active kidney transplant list are from BAME background, with an astonishing 455 of them currently awaiting a kidney transplant at Leeds Teaching Hospitals NHS Trust alone.
Now a ground-breaking research study to reduce health inequalities around live organ donation aims to identify barriers to living donor kidney transplantation for people from black, minority and ethnic (BAME) backgrounds. It will also explore underserved groups from lower socio-economic backgrounds.
The study has been made possible thanks to funding from Leeds Hospitals Charity who have provided almost £50,000 to fund a research fellow, Dr Ahmed, who will lead the project.
There are not enough donors of living organs from BAME backgrounds to meet demand.
“I lost all my freedom after I was diagnosed with kidney disease.” says Min Minhaj.
“My life has turned into one endless hospital appointment. As well as all the check-ups, I need dialysis every second day, for four hours each time.
“Outside the hospital, my life is strictly controlled.
“I can’t travel far because I need to be on hand for dialysis, and everything I eat and drink is monitored. I can’t even have a cup of coffee anymore. I am scared that my dialysis might stop working, or my health will deteriorate, so I might not even be able to have a transplant when a match is found.”
Living donor kidney transplantation (LDKT) is the most effective way to help patients with kidney disease get back to normal life. Kidneys from a living donor can last up to 20 years, compared to just 10 to 12 years from a deceased donor.
Just 14% of living donor kidneys in Leeds come from ethnic minorities.
Dr Sunil Daga, Consultant Nephrologist and Clinical Academic at Leeds Teaching Hospitals NHS Trust, will lead the new research to explore barriers and needs for decision making around living kidney donation in underserved groups.

Dr Daga said: “The initial review I undertook in February 2021 found that there were several barriers to living kidney transplantation from BAME communities.
“We saw that there was a lack of relevant knowledge, fears about the risks of transplantation for the donor, as well as religious, cultural and financial concerns.
“This made me realise we need to do more to raise awareness and tailor resources and support we offer to patients and their families to reassure them that a living kidney transplant would give the best quality of life.”
The research will involve speaking to staff and patients at Leeds and Bradford renal units.
The interview studies will include recipients of kidneys from living and deceased donors, and patients who are currently on the transplant waiting list, focusing on individuals from South Asian backgrounds, non-English language speakers, and lower socioeconomic backgrounds.
Through this study, Dr Ahmed and his team hope to develop comprehensive patient decision support tools, providing a wide range of resources, including information about the options for transplantation and possible outcomes.
It is hoped that the project will help reduce the health inequalities in access to living donor kidney transplantation for people from underserved groups.