
Globally, October is dedicated to raising awareness of breast cancer, which is the most common type of cancer in the UK.
“Around 1 in 7 women will be told they have breast cancer during their lifetime,” says Dr Mamatha Reddy, a Consultant Radiologist at South West London Breast Screening Service.
“Diagnosing breast cancer as early as possible, increases the chance that treatment will be more successful. So, it’s important we all know what to look out for, about breast screening and how to get help.” Dr Reddy adds, “And we need to talk to men, as although it’s much rarer, they can get breast cancer too as everyone has some breast tissue.”
What should I look out for?

“It’s important you know how your breasts normally look and feel,” says Dr Mamatha Reddy.
She adds: “Being familiar with your breasts by checking them regularly, will help you to spot changes that may be signs of breast cancer. It’s generally better to examine yourself after a period, if you have a regular cycle or at around the same time every month if you don’t.”
Pain in the breast is very common, but not usually a sign of breast cancer. One of the first signs could be a lump or area of thickened breast tissue. Dr Reddy explains: “Many people start worrying as soon as they feel a lump, but while many lumps thankfully aren’t cancerous, it’s best to get checked by a doctor.”
You should contact your GP practice if you notice:
- a lump or change in the size or shape of one or both breasts
- a lump or swelling in either of your armpits
- dimpling on the skin of your breasts
- rash on or around your nipple
- discharge from either of your nipples, which may be streaked with blood
- a change in the appearance of your nipple, such as becoming sunken into your breast.
You can find out how to check yourself at www.nhs.uk/common-health-questions/lifestyle/how-should-i-check-my-breasts
Am I at higher risk?
In the UK, breast cancer rates vary amongst women from different backgrounds. Whatever your background, it is important to be aware of the symptoms. Also, while the exact causes of breast cancer aren’t fully understood, some factors may increase the risk of developing it.

“Being female and increasing age are the two most common risks for breast cancer,” says Dr Reddy. 8 out of 10 cases of breast cancer are diagnosed in women over age 50 who have been through the menopause. But younger women and men can get breast cancer too.
If you have close relatives who have had breast cancer or ovarian cancer, you may be at higher risk. Dr Reddy says: “It’s possible for certain genes to pass down from a parent to child. If you’re worried, ask your GP practice for advice and they may be able to refer you for an NHS genetic test. This will tell you if you have inherited one of the cancer-risk genes or if you are at increased risk for any other reason.”
Can I prevent it?
Although research has looked at how breast cancer can be prevented, there are no definite conclusions.
Some studies have suggested regular exercise can reduce the risk of developing breast cancer by almost as much as a third. There may also be benefit in maintaining a healthy weight, having a low intake of saturated fat and lowering your alcohol intake. These actions can also help with general health, and to reduce the risk of conditions such as heart disease, diabetes and some other cancers.
The female hormone oestrogen can sometimes stimulate breast cancer cells and cause them to grow. If you started having periods at a young age and experienced the menopause later than average, you will have been exposed to oestrogen over a longer period of time which may increase your risk. Being overweight causes more oestrogen to be produced by the body, which can increase the risk of some types of breast cancer.
Studies suggest breastfeeding has a small beneficial effect in reducing the risk of developing breast cancer.
Do I need to be screened?
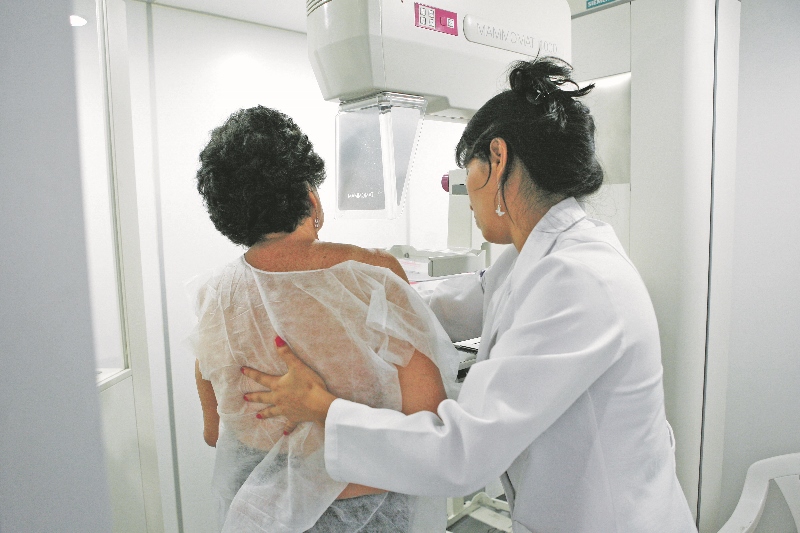
A mammography is an X-ray screening of your breasts. It helps to identify cancers at an earlier stage, sometimes before you can even see or feel any changes to your breasts.
It is offered to women aged from 50 up to their 71st birthday for free by the NHS and prevents an estimated 1,300 deaths from breast cancer each year in the UK. However, Dr Reddy explains that even though we know it saves lives, many women do not feel comfortable coming forward: “Talking to women about what to expect at screening and how we will protect their privacy during the appointment, can help women to feel less anxious.”
The whole appointment lasts around 30 minutes, with the mammogram only taking a few minutes. “You’ll have one or two female mammographers who will explain what will happen and answer any questions you may have. They will do everything they can to make the experience comfortable for you.”
More than two million women a year attend breast screening. Around four in every 100 women need to go back for more tests after screening and out of these four women, one will be found to have cancer.
Most screening appointments will be in the hospital, but if it’s not convenient, some areas offer mobile screening vans in supermarket car parks and other locations. You can contact your local breast screening service to find out where you can get a mammogram in your area.
From the age of 71, the NHS will not send you an appointment, but if you would like to continue breast screening every 3 years, you can call your screening service to request a mammogram.
And don’t worry if you missed an invitation for breast screening, whether it’s weeks, months or even years ago. You can still contact your screening service to arrange your appointment.
We can’t be shy about breast cancer

Usha Marwaha, aged 69 is a former fashion designer and active grandmother to four young children. She is diabetic, a heart patient with two stents and also a breast cancer survivor, as she explains: “In 2009, while watching TV, I felt a twitch in my left breast. As I touched it, I felt a lump. Initially I thought nothing of it but decided to have it checked at my GP practice.
After a biopsy, where a small sample of tissue was taken from the lump for examination, I was diagnosed with stage 4 hormonal breast cancer. Very quickly I started radiotherapy, and thankfully following that, I was 8 years in remission.
In 2017, the cancer reappeared in the same breast. Despite concerns from doctors about whether I could handle surgery due to my other health issues, I had a mastectomy to remove the breast, followed by 8 months of chemotherapy. Thankfully, I was cancer-free again.
In 2020, I returned from a family trip to America and, along with my family, was unwell. COVID had just started spreading across the world and we thought we might have it. As tests didn’t yet exist, we didn’t know for sure.
My family recovered, but I didn’t. As antibiotics didn’t help with my chest infection, my doctor organised a CT scan. I was told that cancer cells had leaked into my lung and spleen.
I have no family history of breast cancer, and being diagnosed with cancer three times in just over ten years has been challenging – mentally, as well as physically. The side effects of chemotherapy and changes in my physical appearance have been really difficult. At one stage, I was told I may only have 9-18 months left to live.
With the continued support of my husband, children, and grandchildren, who say such wonderful things to keep my spirits up, I kept busy and sometimes even forgot my illness. I completed my treatment, attended every test and thankfully, my last two CT scans have shown my cancer has cleared again.
Times can be difficult, but I find strength from within and try to stay positive. I still enjoy art and fashion and learning creative ideas from YouTube. I also get strength from volunteering with South Asian Health Action (SAHA) as I share my story and raise awareness in the local community. Through them, I joined the NHS Core20PLUS5 health inequalities project as a Cancer Community Connector where I can talk to others who have cancer as they understand how I feel.
In our culture, we’re often shy when it comes to our body parts. But we can check ourselves for lumps and bumps, whilst in the shower or when watching TV, like I did. We can take up the offer of cancer screening if we receive a letter in the post. We can contact our GP practice with a list of your questions if something doesn’t feel right. It may turn out to be nothing but can put your mind at rest. And if turns out to be cancer, getting treatment sooner can save our lives.”















